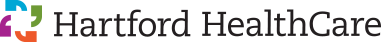Office of the future
HHC embraces the ‘OFFICE OF THE FUTURE’
By Susan McDonald
Well before a pandemic sent most office workers home with their laptops to avoid virus spread, Hartford HealthCare took steps to make workplaces as safe as possible.
David Casale, senior director of facilities planning and construction (left) and Thomas Vaccarelli, VP Facilities, Construction, Real Estate (right) looks over plans for build-out of new offices in the Pearl Street location in Hartford. Changes in office layout and design have resulted from evolving infection control concerns and space utilization trends.
Photo by Chris Rakoczy
Dave Casale, senior director of facilities planning and construction, was months into developing new office space in adjoined buildings at 600-700 Pearl St., in downtown Hartford. Departments are gradually relocating into space designed to leave teams happy and healthy.
It’s part of creating the “office of the future,” a process, Casale said is becoming more detail-oriented every day.
“There is more rigor and intensity on the planning side,” he said.
When working in “live” patient care areas, for example, stringent guidelines ensure patient and colleague safety. Building space for the state’s first proton therapy center, he continued, demanded understanding complex technology.
Pearl Street houses non-clinical teams, so demands differ, influenced heavily by infection control concerns COVID-19 highlighted.
“The pandemic changed everything,” Casale said. “We have to consider whether we are still putting 150 people on a floor as we thought, or plan for the next thing.”
Safe-guarding colleague well-being has always been considered but he said the focus sharpened after the pandemic. Considerations include:
• Air circulation. “We strongly considered infrared filtration like you may see in a clinical environment,” Casale noted.
• How people use space. Pandemic guidelines demanded six feet of space between people. How does that impact walking through an office, or using shared restrooms and kitchens?
• Effective cleaning tactics. “Some degree of anxiety is normal, but it’s about educating people about the environment they’re in,” Casale said. “It’s about finding that comfortable ground between social distancing and efficiency.”
Today’s offices are moving more toward arranging teams in open, collaborative areas instead of offices. This can mean cubicles which “separate people but are not specifically designed to protect them,” he said.
While much-maligned, standard cubicles, when reimagined with features like glass panels, can allow a space to feel larger and colleagues to enjoy light flowing through while being protected.
The Marketing, Communications and Planning departments are planning a move to the Pearl Street complex, and Casale said curving cubicles will carve out space for team members. Colleagues will face different directions, too, increasing privacy, sound efficiency and protection against the spread of germs.
At the Connecticut Orthopaedic Institute’s (COI) new St. Vincent’s Medical Center location, leaders turned to colleagues who will use the space to help decide what it would look like.
“We mocked up a patient room and asked colleagues from nursing, physical therapy, the PAs – everyone who would use the space — to go in and tell us where they’d want the glove dispenser, the white board, the sharps container,” said Elizabeth Maselli, COI operations manager. “We went back to the teams several times to review plans and let them see the progress. It’s their space — they’re the end-users.”
The approach is standard work at the COI, added Andrew Turczak, senior regional director of operations, who noted that physician leadership and doctors “think about every level of the detail, which is truly unique.”
The collaboration yielded requests for motivational artwork on the floors, attention to the proper height of patient chairs and toilets, and signage highlighting the path for patients through the hospital lobby to the COI.
“They put their touch on this project,” Turczak said of the doctors.
The connection has improved staff engagement, according to Maselli.
“We’ve gotten rave patient reviews, but the staff also loves the space. It’s new and they have what they need,” she said.
Adds Karen Platt, COI program manager and a nurse, “A lot of the team has been with orthopaedics for a while and this is a gift as a nurse to have this space to work in. It’s bright and spacious.”
Fresh approach creates fun, inviting work environment
By Susan McDonald
The job can be stressful — helping often distraught callers find needed services across Hartford HealthCare — but what is not stressful is the Access Center environment itself.
Patient service liaisons Chyquan Williams and Amber Weed said the new Access Center is an ideal place to work.
Photo by Chris Rackoczy
It’s no accident — leaders of the new department deliberately cultivated an upbeat, supportive and even fun work life.
“It’s a different culture — I can comfortably speak with my managers. They focus on the work we do, but also on us as people,” said Chyquan Williams, a patient service liaison (PSL) with the Access Center. “Everyone is one here. I’m really happy to go to work every day, even though I have a one-hour commute. That says something!”
Amber Weed, who is also a PSL, added, “It’s fun coming to work — everyone is always happy and comfortable. We all get along and everyone is helpful. It’s like a second home for me — I’m as comfortable here as I am at home.”
They are part of the equation Dr. John Foley, HHC associate vice president of medical affairs and Access Center medical director, crafted for success.
“We have been purposeful about creating an environment where people want to come to work,” he explained. “We ‘hire for smiles’ — patients on the phone know when you’re not smiling. Every potential colleague is interviewed by multiple people. It’s labor intensive, but you can’t take someone who’s not nice and make them nice.”
He spoke from his windowless office while Weed, Williams and other PSLs fielded phone calls in cubicles bathed in sunshine from floor-to-ceiling windows. Office assignments, he said, represent a team investment.
“The most important asset we have is our champions. People should have a good experience here. That’s part of the overall plan,” he said
That plan is tended daily by Access Center Director Michael O’Malley and Manager Theresa Gentile, recruited to start operations August 24, 2020. They oversee about 120 PSLs, with a goal of adding many more.
Access leaders created an open floor concept with larger desks and guidelines protecting those working in person through the pandemic. Working with the building owner, there are limits to the number of people in elevators, break rooms and restrooms, with designated overflow areas on each floor, O’Malley explained.
“The design makes you feel very comfortable — there are lockers that lock, a quiet room and lactation room for new moms,” Gentile explained. “These are not things you have in a traditional office. Everything has been done very mindfully.”
The quiet room helps colleagues regroup after challenging moments on the phone.
“They are often having heart-breaking conversations with people that can knock you out. The room has big, comfy chairs with low lights. Our people need things like that,” Gentile said.
The supportive culture includes fun activities like a birthday club, monthly breakfasts and celebrations when new colleagues finish orientation, she added.
“We do things above and beyond. It’s called ‘The Journey to Yes.’ We’re not allowed to say no, and we’re always approachable,” Gentile said.
Much of it stems from Dr. Foley’s fascination with Walt Disney, an organization known for creating positive work environments. Establishing similar practices helps create a workforce in which colleagues feel valued and value each other, a goal of the system-wide #123 initiative.
The Access Center environment is so positive that when some colleagues worked from home in the pandemic, Dr. Foley said they felt they were missing something. So, he, O’Malley and Gentile brainstormed ways to keep them involved in the fun.
“We have an integrated care team that comes up with ideas to implement. It’s great that they’re willing to do that and make things better,” Williams said.
Medical office traffic flows more smoothly after revamp
By Susan McDonald
COVID rearranged everything that is familiar, including the traffic flow of people through hospitals and medical practices.
Frederick Bailey III, PTA, MBA. East Region director of the HHC Cancer Institute, was instrumental in helping with the process of social distancing and signage in waiting room areas during the COVID-19 pandemic.
Photo by Jeff Evans
While many facilities closed, making visits virtual, hospitals could not and people like Fred Bailey were tasked with maintaining access without endangering the health of colleagues and patients. The East Region director of the Cancer Institute, Bailey tackles planning in the region’s incident command hierarchy.
“It was a big assignment but it was fun and I like a change, especially when it’s for the best,” Bailey said. “We were making a better experience for patients and families, but also for our team, who felt safer.”
As part of pandemic physical distancing guidelines, Bailey’s assignment was to eliminate areas where groups of people congregate, such as when waiting to be seen by a healthcare provider. Instead of waiting in rooms lined with furniture, Bailey’s team tapped LEAN principles to streamline the check-in process for patients. Furniture with upholstery that couldn’t be wiped down was removed, the number of chairs reduced and Plexiglas shields installed.
“They are now more of a ‘greeting room’ than a waiting room,” he said. “It helped us remove that stigma of going to the doctor’s office and having to wait forever in the waiting room. There is no wait.”
A new workflow had to be developed to make this happen. Patients now call or text office staff to announce their arrival. When the office is ready, they are asked to come in. They are met at the door by a practice representative who takes their temperature and brings them into an exam room to be joined by the provider for the visit.
“There were a lot of technical things we had to do — outfit some computers with necessary equipment, teach staff the workflow, collaborate with environmental services and facilities on repurposing chairs. We tried to be fiscally responsible relocating the chairs and created a grid to show what went where,” Bailey explained.
The project involved creating and placing signage, visual cues, elevator posters and floor markings to help people navigate with pandemic restrictions. The efforts touched all offices at Backus and Windham hospitals, as well as the region’s larger off-site locations.
“It was a lot of work but everyone understood it was for their and our safety. The pandemic forced us to be more efficient and some of these changes will be permanent. This is our new normal,” Bailey said.