Every day, our colleagues do amazing things to benefit patients and the community. Email your moments that matter to susan.mcdonald@hhchealth.org.
Natchaug Client Conquers Her Self-sabotaging Ways

Natchaug Hospital’s clients regularly emerge from treatment feeling renewed and able to combat life’s challenges with the tools they are given by staff who are determined to help them heal.
At a recent graduation ceremony, Sarah, a woman from Mystic, told about climbing out of the hole childhood trauma and mental health issues left her in.
“In elementary school, I was usually daydreaming … I would think about living in a home where I had a mom and dad that didn’t always fight, a home where I wasn’t emotionally neglected and given hugs, told I was loved,” she says.
After dropping out of high school and starting to drink, Sarah says she jumped from one job to another. She’d start jobs enthusiastically and eventually self-sabotage herself to the point where she’d quit or get fired.
“It came in the form of criticism from myself in the voice of my abusive past,” she recalls. “I would hear myself say that I was making no difference and the job didn’t make one either.”
“When you come from a home of neglect, you never get nurtured to grow into yourself.”
After being diagnosed with bipolar disorder in her 30s, Sarah tried therapy unsuccessfully. Instead, she’d keep her emotions to herself to avoid shame. She was left struggling with doubt, anxiety and suicidal thoughts.
A new job caring for people with dementia in her 40s left her feeling rewarded and passionate. Yet, old patterns still emerged and the emotional weight caused a breakdown. She finally called Natchaug’s Care Plus Program, where she found others who understand what’s she has gone through.
“When I sat down for my first therapy session, I let out a sigh of relief as other patients began to tell their stories,” Sarah says. “Some of the stories were similar to mine, some not, but the pain we all carried was relatable … I finally felt validated and really began to open up.”
For two months, the program helped her learn to make human connections, and credits Peter DeRosa, her therapist, with helping her learn how to communicate “with guidance and wise correction.”
“I found a new strength in me … and I now look forward to the future as I see a light at the end of my tunnel,” Sarah says.
—Susan McDonald
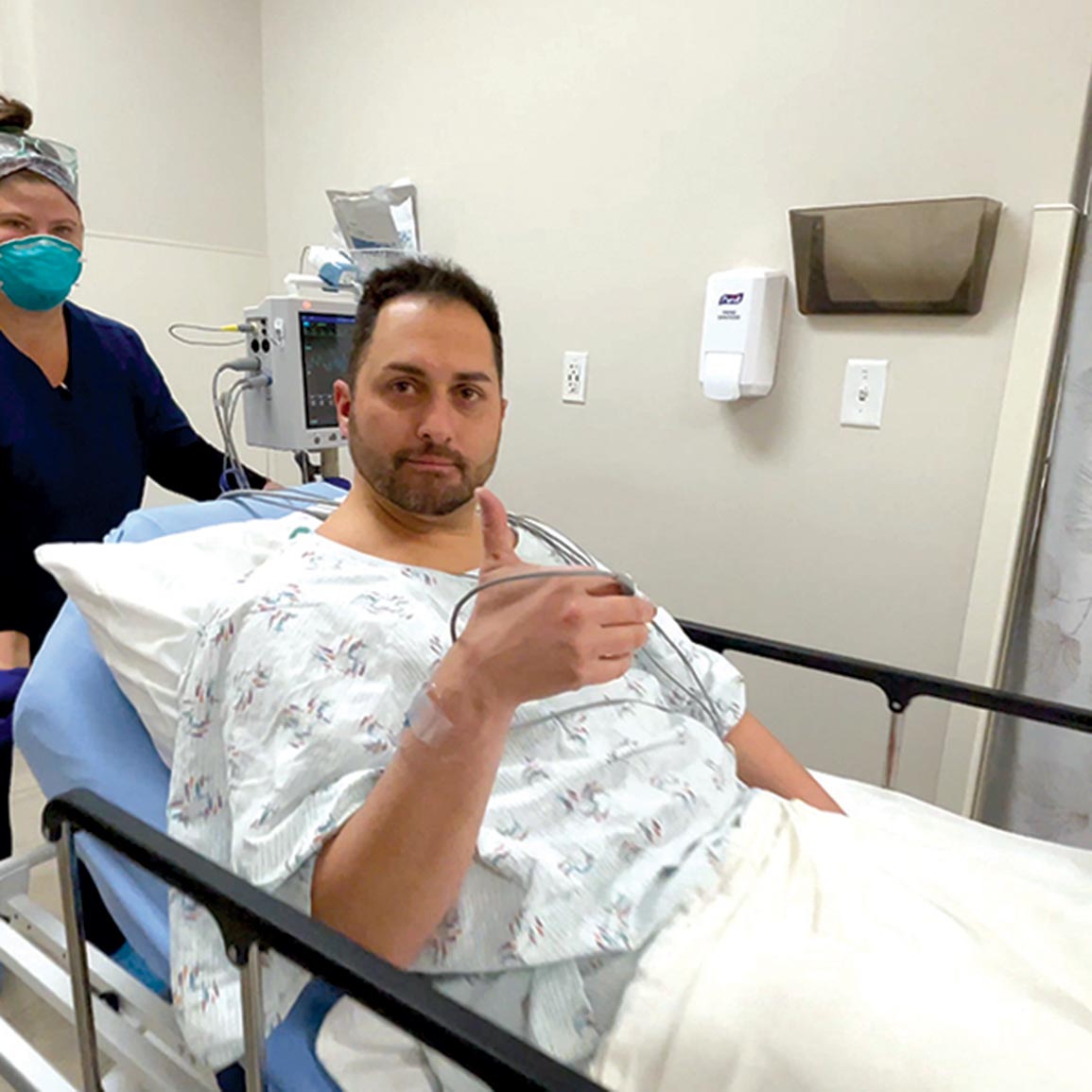
When the Colonoscopy Conversation Gets Personal
In 2019, when I was 37 years old, I went for a routine physical and my doctor discovered something that prompted concern. To err on the side of caution, he wanted me to go for a colonoscopy. In the end, I was completely fine.
However, during the colonoscopy, the doctor found and removed two small polyps from my colon. He then told me if the polyps had stayed in my body until I was 50, which, at the time, was the recommended age to start getting regular colonoscopy screenings for colon cancer, they would have likely turned into cancer. Hearing that gave me chills. The recommendation was for me to get a colonoscopy every three years.
Fast forward to now, studies show more and more people under the age of 50 are being diagnosed with colon cancer. That concerning data prompted the American Cancer Society to change its guidelines, dropping the recommended age for colonoscopies to 45. Of course, people at greater risk are advised to start that screening even sooner. I now fall into that category.
I’ve encountered countless people over the years who continue to put off getting a colonoscopy because they don’t think they need one or they’re afraid because they don’t know what to expect. When I was due for my screening, I thought it the perfect opportunity to show people how it works, what the doctors look for and how life-saving it can be. I hope doing this will help save someone’s life.
—Brian Spyros
Backus Public Safety Officers Begin Carrying Narcan
Members of the Backus Hospital public safety team now carry Narcan, a life-saving medication that can reverse an overdose from opioids — including heroin, fentanyl and prescription opioid medication — in minutes.
The step was prompted by an increase in incidents in which public safety officers are called to help unresponsive individuals in hospital parking lots.
“Carrying naloxone is no different than carrying an epinephrine auto-injector for someone with allergies,” says Gen Boas, director of public safety at Backus and Windham hospitals. “It simply provides an extra layer of protection for those at a higher risk for overdose and gives our team one more tool to help them protect the communities we serve.”
There are two ways to administer Narcan, injecting it into the thigh or leg, and a nasal spray. The Backus team, which includes a K-9, will be the first public safety officers at Hartford HealthCare to carry the medication and will act as a pilot program for other teams throughout the state.
“This initiative was brought forward as an idea from the public safety officers in the field,” explains East Region Vice President of Operations Matt Kaufman. “The public safety team can find themselves as first responders when patrolling the campuses, and, with the unfortunate growth of overdose risk in the community, we saw this as an idea that met a need to benefit patient safety.”
The program will expand to Windham soon, Kaufman adds.
—Ken Harrison
Our Youngest Fan

Ambulances Find New Purpose in Public Health

It’s easy to reuse furniture, clothing, even a car you no longer need. But an ambulance? Turns out that’s pretty easy, too.
Four ambulances retired from service at Hunter’s Ambulance Service found new life helping others in new ways, says Kevin Ferrarotti, senior system director for Hartford HealthCare’s emergency medical services and administrative director of Hunter’s, part of HHC’s system of care.
One will be part of the HHC Neighborhood Health initiative, which brings health prevention services and support directly to people and communities across the state. Neighborhood Health teams stage clinics in locations like community centers, soup kitchens and shelters to provide medical care to underserved populations.
“I love this, it’s such a great use,” Ferrarotti says. “Currently, all the supplies and consumables they use for Neighborhood Health are transported in different vehicles. Going forward, they will use the repurposed ambulance to transport everything they need.”
The ambulance was stripped of all emergency lights and sirens and branded with HHC and Neighborhood Health logos, says Kelly Toth, APRN, system clinical director of Neighborhood Health. Fully stocked with food, snacks, hygiene products, clothing, blankets and medical supplies, it will also have barber supplies on hand as Hartford barber Miguel Delvalle often works with the team.
“This was one of our longer-term goals, and to have it come to fruition is incredible,” Toth says. “We will quite literally be meeting people where they are in the community.”
Ferrarotti and Toth say the goal is to eventually have one repurposed and branded ambulance in Neighborhood Health regions across Connecticut. This first will stay in the Hartford Region.
Two other ambulances are mobile training units, one each for the University of New Haven and Hunter’s. Hunter’s “will be the only ambulance company in the state to have a true mobile simulation ambulance,” Ferrarotti says. “It will be used in EMT and paramedic training and as a recruitment tool.”
The fourth ambulance went to Rushford, a Hartford HealthCare provider of addiction and mental health services, for opiate awareness and prevention programs through the Meriden Opioid Referral for Recovery (MORR) project and others. The collaboration between Rushford, City of Meriden and Meriden first responders focuses on addressing the opioid crisis through Narcan administration in the field and referrals to specialized MORR staff embedded on Rushford’s Crisis Team. The program is a way for people to receive the treatment they need rather than being incarcerated.
“The ambulance will help people have a greater sense of privacy at these programs,” Ferrarotti says.