Sharing the CARE with Colleagues
By Haley Guidotti
The Hartford HealthCare Access Center leadership team strives to provide a fun, engaging work environment, including creation of the CARE Team to promote a positive, interactive experience in their office.
Standing for Compassionate Associates Recognizing Everyone, the group is led by Access Center patient service liaisons (PSLs). It started as a way to provide colleagues an opportunity to organize various activities and themes for everyone to enjoy. They meet weekly to propose, plan and execute monthly activities, giving PSLs a way to collaborate and share ideas freely before bringing them to leadership.
Thanks to the CARE Team, PSLs says they look forward to dress-up days and different activities at the office, located on Pearl Street in Hartford.During Pride Month, for example, the team directed colleagues from different departments to wear different colors so, together, they created a human rainbow.
Late last summer, the team implemented aCARE Cart which moves throughout the various departments each day, providing PSLs different items to help brighten their day and relieve any stress. Items in the cart include mints, essential oils and stress balls.

Superhero Returns to Running
By Brian Spyros

As chief of emergency medicine at The Hospital of Central Connecticut (HOCC), David Buono, MD, is used to taking care of others but, over the past year, he had to unexpectedly take care of his own health.
In October 2021, the 60-year-old was diagnosed with prostate cancer after a routine PSA.
“I skipped the PSA test the last few years because I thought everything was fine,” Dr.Buono says.
Last February, he underwent robotic surgery at HOCC to remove his prostate and, ultimately, the cancer. Dr. Buono, who admittedly doesn’t like to sit still, found it challenging to get back to one of his passions — running.
I was slower and sore after surgery. I had to build up my endurance to run again and really learn to pace myself,” he explains.
Before surgery, Dr. Buono had signed up for the 2022 Hartford Marathon, an event he’s run for 20 years. He wasn’t going to let his cancer diagnosis stop him.
“I wanted the race to be my focus, not the cancer,” he says. Over the seven months leading up to the marathon, he worked hard to get back in shape — preparing for the big day.
At the same time, Dr. Buono was one of a handful of runners chosen to join the Hartford Marathon Foundation’s 2022 Inspiration Team, which highlights runners for their strength and resilience in the face of adversity.
He used the opportunity to remind others about the importance of routine health screenings, especially when it comes to cancer.
“I want people to understand that these types of screenings are so important. I had no symptoms prior to my cancer diagnosis, so if it wasn’t for the blood test, I would’ve never known,” Dr. Buonosays. “I am on a mission to get the word out about screenings for various types of cancers. We have them for a reason and they save lives.”
He successfully ran the Hartford Marathon in October, placing eighth in his age group, to continue what’s become a yearly tradition.
“My goal is to be the oldest person running this race one day,” Dr. Buono says with a smile.
Innovative LIFE STAR Nurse Earns Leadership Award
By Kate Carey-Trull
Heather Standish was honored with the 2022 Doris Armstrong Leadership Award, the first given since Armstrong’s passing last winter.
For 32 years, Hartford Hospital has given out the award to honor Armstrong’s legacy as vice president of nursing there from 1976 to 1990. Nursing leaders who embody her visionary, high-energy and caring leadership style are chosen for the award.
Standish joined the LIFE STAR team in 2007, progressing from a novice flight nurse to the current nurse director. Her colleagues described her as a true advocate for her patients and authentic in her interactions with staff. She encourages staff to grow and take on projects and leadership behaviors, and provides support and guidance.
Starting as a paramedic in 1995, Standish became a nurse, first working at Backus Hospital before transferring to Hartford Hospital in 2003. At Hartford Hospital, she worked on the cardio thoracic floor and cardiothoracic ICU. All of these experiences prepared her for her dream job of becoming a LIFESTAR flight nurse.
At LIFE STAR and Hartford Hospital, Standish has made significant innovative contributions to the nursing profession. She spearheaded a project enabling LIFE STAR to carry blood products on the helicopters, partnering with Hartford Hospital’s transfusion team leadership and LIFE STAR’s medical director to develop and implement a well-developed process. The project has helped more than 100 critically ill and injured patients, and earned the team a Full Circle Award and Standish a Nightingale Award for Excellence in Nursing.
Holder of numerous certifications, Standish is leading her team in hosting a “Fundamentals of Critical Care Conference.”

Robotic Hernia Repair Makes Patient’s Recovery Easy
By Elissa Bass
For about six years, Thomas Ottone left his hernia untreated; it got worse, larger and more painful until it became debilitating.
He finally went to see general surgeon Chike Chukwumah, MD.
“He came to me with a bilateral complexing uinal scrotal hernia,” Dr. Chukwumah recalls, adding that, left untreated, a hernia like this can be life-threatening.
Because Ottone’s hernia — which starts as a defect in the abdominal wall muscle — grew so large, his large intestine basically moved into it, becoming trapped.
More complicated
To repair the hernia, Dr. Chukwumah had to put the large intestine back in what he called its “natural anatomical location.” The surgery was tricky, because the large intestine hadn’t been in its proper location for some time, and moving it back could have repercussions elsewhere, especially with the lungs, he says. It was important to make sure the move wouldn’t put pressure on Ottone’s lungs, causing respiratory distress.
“We talked about not doing both sides at once,” Dr. Chukwumah says.
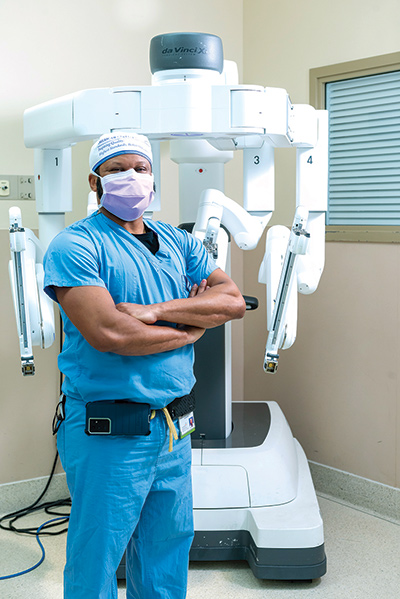
Having a robotic surgery option prompted the decision to take care of the entire hernia at once.The robot in the Hartford Hospital operating room gave Dr. Chukwumah the precision needed to safely repair the hernia and push the large intestine back in place, which he did in a five-hour procedure.
Because the procedure was robotic and required only five one-inch incisions on his abdomen, Ottone was discharged the next day, and only needed a few days of over-the-counter pain management.
Robotic was the best option
“I also do these surgeries laparoscopically, which is also minimally-invasive, but the robot has made these surgeries certainly easier,” Dr. Chukwumah notes. “The other option would have been a laparotomy (surgical incision into the abdominal cavity), which is a big incision. With that, you are looking at three to five days in the hospital. It’s a painful surgery, so the recovery can be challenging.”
Calling the robot a “game changer” for such procedures, he says, “There is a much lower hernia recurrence with the robot, greatly reduced postoperative complications, functional recovery happens in a quarter of the time, and pain management is non-narcotic.”
Two months after surgery, Ottone felt “back to normal,” driving and moving well and without pain.
“I feel so much better,” he reports. “I shouldn’t have waited.”